All done!
#thankyou
#BoxyOut
10 months ago today, on Friday September 18th, I was in the shower getting ready for a night out in Hamburg, when I found a lump in my left breast.
I saw my GP at 8am on the Monday morning and was in hospital three days later. I had a consultation and was then sent upstairs for a mammogram, ultrasound and biopsy. By the time I was back downstairs with the consultant, she had most of the results and told me it was highly likely I had breast cancer. I was in and out of the hospital in 90 minutes. That was my Thursday.
The next day, I went back to the UK for a wedding and caught up with a heap of friends, all saying ‘Haven’t seen you in ages! How are you? How’s Amsterdam?!‘ totally unaware of what was about to drop. I spent that weekend getting my head around it all, before returning to Amsterdam to have it confirmed that I had a triple negative tumour in my left breast.
Monday September 26th – that was diagnosis day.
On that day, I asked a lot of questions. Can I still work? Can I still travel? What treatment do I need? How long will is last? Will I be hospitalised? Do I have to go back to the UK? Ultimately, what I was getting at was ‘if I give this thing every ounce of strength, focus, and determination I have, how long do I need to put my life on hold?‘
I was told treatment would last 9-10 months.
I started treatment five weeks later (delayed two weeks at my request, so I could finish my F1 season in style at the US GP in Austin, Texas!) and had my first chemotherapy session on Monday October 31st.
Since then, I’ve had two rounds of chemotherapy, lumpectomy surgery, removal of six lymph nodes, and I’m now having daily radiotherapy.
My final treatment is scheduled for Wednesday July 26th 2017 – exactly 10 months since I was diagnosed; but 8 months, 4 weeks, 2 days after I started treatment.
We’re finishing 5 days ahead of plan – Boom!
In many ways, it’s been a life-changing journey. But all I can think of is getting back to normal. I will need to take tablets every day for the next five years, and have regular check-ups for the next ten years. But aside from that, there’s no reason why I can’t lead a normal life.
The tumour is gone. It hadn’t attached itself to the tissue around it. And the scar on my left breast is neat, tidy and will be my reminder of this great battle.
My lymph nodes were clear, confirming that the cancer hadn’t spread beyond my breast. The wound under my left arm is healing and is now giving me a focus for my training – to regain full movement in my left shoulder/chest and rebalance the strength across both shoulders.
The likelihood of my cancer coming back is 10-15%. But if 1 in 3 people will get it at some point in their lives, then Joe Public has a 33% chance, so I’m no worse off than anyone else reading this blog!
So on that note, I’m now just focusing on the next eight days, six treatments, then taking a long weekend to go to my first F1 race of the season – my ‘comeback’ race, perfectly timed!
And on Tuesday August 1st, life begins again… Bring. it. On.
#startstrongfinishstronger
#kickedcancerouttheballpark
#wearestrongerthancancer
#BoxyOut
By now, most people will probably have got used to me sharing the detail, bearing all, and going geeky on the science behind all this! Well last week, I had a meeting with the Radiologist and she gave me a little more insight into what they’re doing to me in phase 3.
Because the area to be radiated (the radiation ‘field’) is in my left breast (directly in front of my heart), we use a technique called ‘breath hold’ – this literally means I hold my breath during radiation, so my lungs expand and push my heart back away from the radiation ‘field’. In the clip below, the Radiologist explains how this works, using the scans they took of my chest…
In my last post, I included a couple of photos of the treatment room, where I lie down on a bed, with my arms above my head, while the machine moves around me and zaps my chest from various angles. The graphic below shows the various angles from which I am treated. In each image, the radiation field is in between the parallel lines. As the graphics build up, the intensity of radiation builds in the specific area where my tumour was located. So you can clearly see how targeted this treatment is (in comparison to chemo, which went around my whole body).
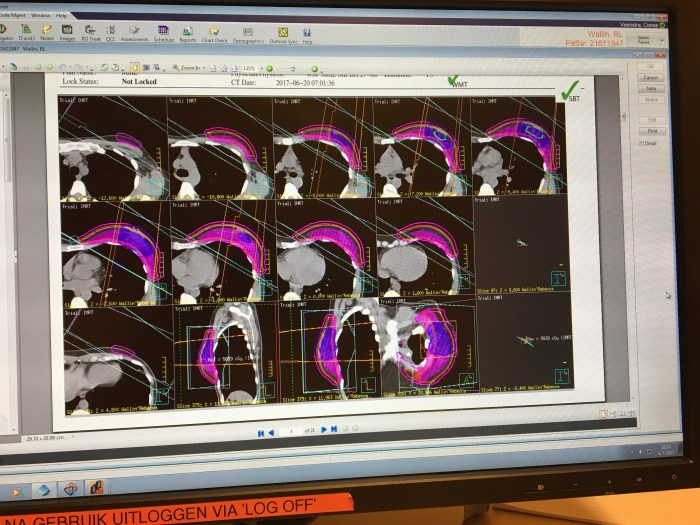
During each zap, the noise the machine makes is defined by the shape of the radiation field. This isn’t just a straight beam, it is shaped by many individual plates which come into the radiation field – a bit like the gadget you put your hand into to make an imprint…

Before each scan, these metal plates move until they outline the required shape, and the radiation is then beamed through that shape to radiate the precise area in my breast.
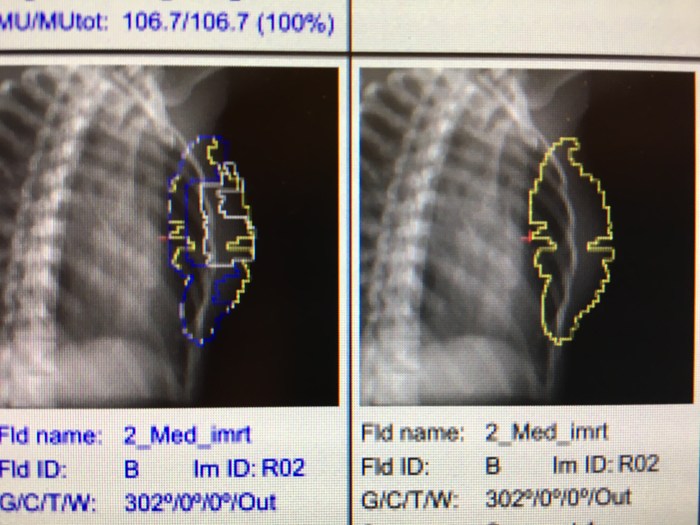
I find this stuff super interesting, and it really helps me understand what the machine is doing while I’m lying there. It all takes less that 3 minutes and I don’t feel a thing!
In the same way that we have to protect my heart during radiation, with other forms of cancer, they also have to take specific precautions to protect other major organs. In this case, I feel lucky my tumour was in an area which is easy to get at, as the precautionary measures are pretty simple – just hold your breath.
But I still feel like James Bond every time I lie on the machine 🙂
OK so we gave up waiting for the axilla wound to heal (that’s still ongoing!) and this week I started the third and final phase of my treatment – radiotherapy.
Some people do this bit first, some people just do this bit and nothing else. But for me, it feels like a nice way to finish treatment, because it should be the easiest. That means I can start getting my life back to normal while I’m having treatment!
One month to go
A week before I start having my treatment, I’m invited to meet the Radiotherapist, Dr Russell. This feels a bit weird; she’s been involved in my treatment for the past eight months and knows more about me than I do! At each stage of treatment, where a decision has been made, the team looking after me (Oncologist, Surgeon, Pathologist and Radiotherapist) have planned things collaboratively, to ensure that whatever treatment I’m given is the best thing for me at the time, in the context of what’s still to come and what’s gone before. This sounds logical, but it’s still reassuring to know that they’re all working together to get me fixed.
So I meet Dr Russell and she explains what’s going to happen during my treatment. Today I’ll be ‘prepared’ then my treatment will start about a week later. Treatment will be 21 sessions, once a day, Monday-Friday. In my usual way, I ask plenty of questions – can I work? Yes. Can I train? Yes, that’s actually recommended as it’ll give you more energy, just go easy! Cool! So what are the side effects? Tiredness, itchy skin, sensitivity, oh and a very small chance of heart failure… WHAT?! It turns out that, because my tumour was in my left boob and my heart sits directly behind it, they need to make sure they don’t zap my heart! But they’re not too worried; apparently, breathing in fills my lungs and pushes my heart back away from the area being zapped – simple! So as long as I can hold my breath for 40 seconds I’m fine! Erm, OK, if you say so…!
Dr Russell reassures me that this really is nothing to worry about, and I’m sent off to be ‘prepared’.
Boob art
Whenever I’ve mentioned radiotherapy to anyone who’s been through it, they all seem to ask if I’ve had my tattoos yet? Surely they’re not serious? Oh yes, they are! The ‘preparation’ involves a quick CT scan, then letting the nurses loose on my chest with felt tip pens, ink and a tattoo needle!
First up, they do a CT scan to get a detailed picture of the inside of my boob. Next, they lay me down on the radiotherapy machine, and line me up so that the lasers will zap me in exactly the right place. While I’m on the machine, it shines green guidelines onto me (like when you use a laser to point at a presentation screen). The nurses then draw on my chest with felt tip pens to mark where the laser grid lines are, so that when I come back next week, they can line me up in exactly the same position. Makes sense, but what if the felt tip rubs off in the shower? That’s where the tattoos come in! Where the grid lines cross, they tattoo tiny dots on my skin, so that I can always be lined up in the same place. They’re only tiny and look like freckles, but they will be permanent.
I actually find this all quite entertaining, especially when they give me a pen and ask me to keep my lines ‘topped-up’ until next week… How am I meant to do that? I can’t see half the lines, let alone draw them on myself! Luckily for me, I’m heading to London for the weekend… Once again, enter Nurse Kari…
So Kari, what did you do at the weekend? Ah not much, just drew all over my mate’s boobs in felt tip pen… as you do… We had a few attempts at it, because she kept giggling and I was ticklish! I was half expecting to see a Banksy or some crude graffiti when I looked in the mirror, but luckily Kari kept her artistic flair at bay and I was back to looking like a walking Ordnance Survey map.
Treatment begins…
Many people have asked why I chose to have treatment in the Netherlands rather than back home in the UK. Well, everyone who’s been over to help me in the past eight months has seen the facilities over here and experienced the efficiency and friendliness of the team looking after me. Clearly, I’ve never experienced cancer treatment in the UK, but based on the facilities alone, there’s just no comparison.
Unlike chemotherapy and surgery (which were both at the OLVG hospital in east Amsterdam), radiotherapy is at the Dutch Cancer Institute (AVL) in the west. I was impressed by the OLVG, as it never felt much like a hospital, and the people were all super friendly. Well the AVL is much the same.
AVL (Antoni van Leeuwenhoek) is a hospital in the Netherlands, which specializes in the diagnosis and treatment of cancer. It feels more like a shopping mall than a hospital, and the layout and facilities are just first class. The atmosphere is laid back, there’s a library, an internet café, a museum, and they even sell beer and wine in the cafeteria! They also have people walking around with trolleys offering tea and coffee to whoever is sitting around – patients, friends or family; if you want a drink, they just hand it out. It all feels very relaxed.
My own private retreat
So on Tuesday, I arrived for the first of my 21 sessions. By this point, I was relaxed and had a good idea of where I was going, and what to expect:
The radiation area is one big room, with diving walls coming in from each side to divide it into an S shape. At the top is the area where the nurses sit, then there’s a corridor and on the other side is the large area where the radiation machine is. There are cameras, speakers and microphones all around the machine, so the nurses can see and hear me from their area, and can talk to me and operate the machine without being in direct contact with the radiation themselves. It all sounds very technical, and it probably is! But it doesn’t feel it when you’re in there.
On the contrary, it actually feels more like a spa! Apart from the nurses’ area with their tv screens, the rest of the area is decorated in a really modern and relaxing way – there are uplighters on the floor, script writing on the walls, images of beaches and forests, mood lighting, and sound effects like birds tweeting, waves, branches blowing in the breeze etc. And as you come in, the patients are able to select the theme for all the lighting and sound (the themes are named after locations; so far I’ve tried Australia, South America and the Seychelles?!)
I really like all this; not because it’s cool or spiritual, but because they’ve made a conscious effort to make patients feel relaxed, give them something to do, a choice they can make, rather than just feel like this is all being done to them. It’s a really nice touch and the whole experience feels, almost enjoyable?!
You expect me to talk?
So my visions of lying on a bed with lasers zapping me – as per James Bond and Goldfinger – weren’t actually that far off! I’m lying on my back with my hands above my head. There’s a rest beneath my knees (for comfort) and rests above my head to support my arms and wrists. The equipment then moves around the bed and ‘zaps’ me from specific angles.
In my case, there are four zaps – one from behind my left side (coming at my boob from under my left arm), one from directly above, and two from above my right boob (coming at it diagonally from above). Each zap lasts between 10 and 30 seconds, during which time I hold my breath.
The nurses set me up on the bed, line me up so my grid lines match up with the lasers on the machine, then they toddle off to their area around the corner and talk to me over the tanoy. They talk to me every step of the way, so I always know what’s going on:
After the four zaps are done, that’s it. The machine slides back and the nurses come back and help me up. I get dressed and they smile and say “see you tomorrow!”
It all sounds too easy…
Given the complexity of the equipment, the seriousness of the task in hand, and the journey I’ve been on to get here, it seems flippant to say this, but it’s effortless! I know I’m only four treatments in, and have another 17 to go, but so far all I’ve felt is a little bit tired. And it’s not tiredness like I felt in chemo (that was more like fatigue, energyless achiness) – this is more like I could just hit the sack and sleep a bit more.
But it’s not stopping me doing anything. On Tuesday, I went to work for ive hours before treatment; on Wednesday, I went to the gym for 30 minutes after treatment; on Thursday, I went to work for eight hours after treatment; and on Friday I went to work for six hours before treatment… So I’m working part-time, I’m doing a little bit in the gym, and I’m sleeping like a baby the rest of the time!
OK so it’s not all rosy – my limbs and joints still seize up if I sit still for more than ten minutes, but I’m hoping that will go in time, especially as I start to rebuild my strength and flexibility. My shoulders are painful (from sleeping in odd positions after surgery, and overcompensating by using my right side for everything while my left side was healing). And my feet still ache like hell from the damage of the TC chemo (they’ve said this may improve but may stay long-term). But I’m going to ask about physio to help all this and hopefully I’ll get most of this back to normal in time.
In the meantime, today and tomorrow are rest days, before treatment starts again on Monday with session 5…
#BoxyOut